Research Program

Leadership
Helen Lavretsky, MD, MS
Professor of Psychiatry
Contact Info
Late-life Mood, Stress, and Wellness Research Program Website
760 Westwood Plaza
Rm 37-456
Los Angeles, CA
(310) 794-4619
latelifewellness@mednet.ucla.edu
About
Sadness of cognitive decline are not a normal part of aging. Our program is dedicated to prevention of mood and cognitive disorders and chronic pain in aging, by promoting brain health and wellness. Medical studies have already shown that exercise and mind body therapies such as yoga and Tai Chi, can help to reduce depression in seniors and improve their quality of life. To find the best ways to prevent and treat depression, researchers at UCLA are requesting participants for current medical studies.
“Many seniors and their caregivers are faced with lots of stress, including economic downturns and multiple medical conditions. They can’t always afford expensive medical treatments,” said Helen Lavretsky, MD, professor at UCLA who specializes in geriatric psychiatry and mind-body intervention. “I want to use everything available to promote wellness in seniors and their caregivers.”
Research
Previous research addressed the impact of medical illness and cerebrovascular disease, and candidate genes on cognitive and mood disorders in later life that can alter treatment response and serve as risk factors for future dementia. We have a constantly evolving portfolio of projects, and many require volunteers to participate. Please review our list of studies currently looking for participants.
Published Research
Lavretsky H. Yoga and Meditation Can Help Improve Cognitive Functioning in Older Adults With Mild Cognitive Impairment and Dementia. Am J Geriatr Psychiatry. 2018 Nov 22. pii: S1064-7481(18)30570-0. doi: 10.1016/j.jagp.2018.11.002. [Epub ahead of print] PubMed PMID: 30538073.
Vasudev A, Torres-Platas SG, Kerfoot K, Potes A, Therriault J, Gifuni A, Segal M, Looper KJ, Nair V, Lavretsky H, Rej S. Mind-Body Interventions in Late-Life Mental Illnesses and Cognitive Disorders: A Narrative Review. Am J Geriatr Psychiatry. 2018 Nov 3. Pii: S1064-7481(18)30541-4. doi: 10.1016/j.jagp.2018.10.020. [Epub ahead of print] PubMed PMID: 30527963.
Chang DD, Eyreeuro HA, Abbott R, Coudreaut M, Baune BT, Shaman JA, Lavretsky H, Lenze EJ, Merrill DA, Singh AB, Mulsant BH, Reynolds CF 3rd, Müller DJ, Bousman C. Pharmacogenetic guidelines and decision support tools for depression treatment: application to late-life. Pharmacogenomics. 2018 Nov;19(16):1269-1284. doi: 10.2217/pgs-2018-0099. PubMed PMID: 30422065.
Laird KT, Lavretsky H, Wu P, Krause B, Siddarth P. Neurocognitive Correlates of Resilience in Late-Life Depression. Am J Geriatr Psychiatry. 2019 Jan;27(1):12-17. doi: 10.1016/j.jagp.2018.08.009. Epub 2018 Aug 25. PubMed PMID: 30262406; PubMed Central PMCID: PMC6298796.
Laird KT, Lavretsky H, St Cyr N, Siddarth P. Resilience predicts remission in antidepressant treatment of geriatric depression. Int J Geriatr Psychiatry. 2018 Dec;33(12):1596-1603. doi: 10.1002/gps.4953. Epub 2018 Jul 23. PubMed PMID: 30035325; PubMed Central PMCID: PMC6246780.
Vlasova RM, Siddarth P, Krause B, Leaver AM, Laird KT, St Cyr N, Narr KL, Lavretsky H. Resilience and White Matter Integrity in Geriatric Depression. Am J Geriatr Psychiatry. 2018 Aug;26(8):874-883. doi: 10.1016/j.jagp.2018.04.004. Epub 2018 Apr 23. PubMed PMID: 29803529; PubMed Central PMCID: PMC6086733.
Leaver AM, Yang H, Siddarth P, Vlasova RM, Krause B, St Cyr N, Narr KL, Lavretsky H. Resilience and amygdala function in older healthy and depressed adults. J Affect Disord. 2018 Sep;237:27-34. doi: 10.1016/j.jad.2018.04.109. Epub 2018 Apr 25. PubMed PMID: 29754022; PubMed Central PMCID: PMC5995579.
Lavretsky H, Abbott R. Community-Based Acupunch Exercise Program Improves Physical Health and Quality of Sleep in Taiwanese Older Adults. Am J Geriatr Psychiatry. 2018 May;26(5):521-522. doi: 10.1016/j.jagp.2018.01.207. Epub 2018 Feb 8. PubMed PMID: 29526545.
Abbott R, Chang DD, Eyre HA, Bousman CA, Merrill DA, Lavretsky H. Pharmacogenetic Decision Support Tools: A New Paradigm for Late-Life Depression? Am J Geriatr Psychiatry. 2018 Feb;26(2):125-133. doi: 10.1016/j.jagp.2017.05.012. Epub 2017 May 25. Review. PubMed PMID: 29429869; PubMed Central PMCID: PMC5812821.
Laird KT, Paholpak P, Roman M, Rahi B, Lavretsky H. Mind-Body Therapies for Late-Life Mental and Cognitive Health. Curr Psychiatry Rep. 2018 Jan 25;20(1):2. doi: 10.1007/s11920-018-0864-4. Review. PubMed PMID: 29372339.
Laird KT, Lavretsky H, Paholpak P, Vlasova RM, Roman M, St Cyr N, Siddarth P. Clinical correlates of resilience factors in geriatric depression. Int Psychogeriatr. 2018 Jan 16:1-10. doi: 10.1017/S1041610217002873. [Epub ahead of print] PubMed PMID: 29335041; PubMed Central PMCID: PMC6047931.
Lavretsky H. Complementary, Alternative, and Integrative Medicine Use is Rising among Aging Baby Boomers. Am J Geriatr Psychiatry. 2017 Dec;25(12):1402-1403. doi: 10.1016/j.jagp.2017.08.004. Epub 2017 Aug 30. PubMed PMID: 28939285.
Yang H, Leaver AM, Siddarth P, Paholpak P, Ercoli L, St Cyr NM, Eyre HA, Narr KL, Khalsa DS, Lavretsky H. Neurochemical and Neuroanatomical Plasticity Following Memory Training and Yoga Interventions in Older Adults with Mild Cognitive Impairment. Front Aging Neurosci. 2016 Nov 21;8:277. PubMed PMID: 27917121; PubMed Central PMCID: PMC5116460.
Acevedo BP, Pospos S, Lavretsky H. The Neural Mechanisms of Meditative Practices: Novel Approaches for Healthy Aging. Curr Behav Neurosci Rep. 2016;3(4):328-339. Review. PubMed PMID: 27909646; PubMed Central PMCID: PMC5110576.
Lenze EJ, Ramsey A, Brown PJ, Reynolds CF 3rd, Mulsant BH, Lavretsky H, Roose SP. Older Adults’ Perspectives on Clinical Research: A Focus Group and Survey Study. Am J Geriatr Psychiatry. 2016 Oct;24(10):893-902. doi: 10.1016/j.jagp.2016.07.022. PubMed PMID: 27591916; PubMed Central PMCID: PMC5026966.
Arandjelovic K, Eyre HA, Lavretsky H. Clinicians’ Views on Treatment-Resistant Depression: 2016 Survey Reports. Am J Geriatr Psychiatry. 2016 Oct;24(10):913-7. doi: 10.1016/j.jagp.2016.05.010. PubMed PMID: 27591914.
Lavretsky H. Lifestyle Medicine for Prevention of Cognitive Decline: Focus on Green Tea. Am J Geriatr Psychiatry. 2016 Oct;24(10):890-2. doi:10.1016/j.jagp.2016.08.002. PubMed PMID: 27591162.
Hsu JH, Mulsant BH, Lenze EJ, Karp JF, Lavretsky H, Roose SP, Reynolds CF 3rd, Blumberger DM. Impact of Prior Treatment on Remission of Late-Life Depression with Venlafaxine and Subsequent Aripiprazole or Placebo Augmentation. Am J Geriatr Psychiatry. 2016 Oct;24(10):918-22. doi: 10.1016/j.jagp.2016.04.015.PubMed PMID: 27538352; PubMed Central PMCID: PMC5026879.
Merrill DA, Siddarth P, Raji CA, Emerson ND, Rueda F, Ercoli LM, Miller KJ, Lavretsky H, Harris LM, Burggren AC, Bookheimer SY, Barrio JR, Small GW. Modifiable Risk Factors and Brain Positron Emission Tomography Measures of Amyloid and Tau in Nondemented Adults with Memory Complaints. Am J Geriatr Psychiatry. 2016 Sep;24(9):729-37. doi: 10.1016/j.jagp.2016.05.007. PubMed PMID: 27421618; PubMed Central PMCID: PMC5003686.
Eyre HA, Yang H, Leaver AM, Van Dyk K, Siddarth P, St. Cyr N, Narr K, Ercoli L, Baune BT, Lavretsky H. Altered resting-state functional connectivity in late-life depression: A cross-sectional study. J Affect Disord. 2016 Jan 1;189:126-33. doi:10.1016/j.jad.2015.09.011. Epub 2015 Sep 28. PubMed PMID: 26433760; PubMed Central PMCID: PMC4640990.
Eyre H, Baune B, Lavretsky H. Clinical Advances in Geriatric Psychiatry: A Focus on Prevention of Mood and Cognitive Disorders. Psychiatr Clin North Am. 2015 Sep;38(3):495-514. doi: 10.1016/j.psc.2015.05.002. Epub 2015 Jun 26. Review. PubMed PMID: 26300035; PubMed Central PMCID: PMC4548274.
Eyre HA, Eskin A, Nelson SF, St. Cyr NM, Siddarth P, Baune BT, Lavretsky H. Genomic predictors of remission to antidepressant treatment in geriatric depression using genome-wide expression analyses: a pilot study. Int J Geriatr Psychiatry. 2015 Oct 15. doi: 10.1002/gps.4356. [Epub ahead of print] PubMed PMID: 26471432.
Lavretsky H, Reinlieb M, St. Cyr N, Siddarth P, Ercoli LM, Senturk D. Citalopram, Methylphenidate, or Their Combination in Geriatric Depression: A Randomized, Double-Blind, Placebo-Controlled Trial. Am J Psychiatry. 2015 Feb 13:appiajp201414070889. PubMed PMID: 25677354.
Brown FW. Resilience and Aging: Research and Practiceby Helen Lavretsky, M.D., M.S. Baltimore, Johns Hopkins University Press, 2014, 272 pp., $44.95. Am J Psychiatry. 2015 Feb 1;172(2):204. doi: 10.1176/appi.ajp.2014.14111392. PubMed PMID: 25640940.
Irwin MR, Olmstead R, Carrillo C, Sadeghi N, Breen EC, Witarama T, Yokomizo M, Lavretsky H, Carroll JE, Motivala SJ, Bootzin R, Nicassio P. Cognitive behavioral therapy vs. Tai Chi for late life insomnia and inflammatory risk: a randomized controlled comparative efficacy trial. Sleep. 2014 Sep 1;37(9):1543-52. doi:10.5665/sleep.4008. PubMed PMID: 25142571
Varteresian T, Lavretsky H. Natural products and supplements for geriatric depression and cognitive disorders: an evaluation of the research. Curr Psychiatry Rep. 2014 Aug;16(8):456. doi: 10.1007/s11920-014-0456-x. PubMed PMID:24912606
Reinlieb M, Ercoli LM, Siddarth P, St Cyr N, Lavretsky H. The Patterns of Cognitive and Functional Impairment in Amnestic and Non-amnestic Mild Cognitive Impairment in Geriatric Depression. Am J Geriatr Psychiatry. 2013 Nov 5. pii: S1064-7481(13)00398-9. doi: 10.1016/j.jagp.2013.10.010. [Epub ahead of print]PubMed PMID: 24315561.
Siddarth D, Siddarth P, Lavretsky H. An observational study of the health benefits of yoga or tai chi compared with aerobic exercise in community-dwelling middle-aged and older adults. Am J Geriatr Psychiatry. 2014 Mar;22(3):272-3. doi: 10.1016/j.jagp.2013.01.065. Epub 2013 May 2. PubMed PMID: 23642461
Chen ST, Siddarth P, Saito NY, Rueda F, Haight T, Ercoli LM, Miller KJ, Lavretsky H, Barrio JR, Bookheimer SY, Small GW, Merrill DA. Psychological well-being and regional brain amyloid and tau in mild cognitive impairment. Am J Geriatr Psychiatry. 2014 Apr;22(4):362-9. doi: 10.1016/j.jagp.2012.09.002. Epub 2013 Mar 26. PubMed PMID: 23567426
Abbott R, Lavretsky H. Tai Chi and Qigong for the treatment and prevention of mental disorders. Psychiatr Clin North Am. 2013 Mar;36(1):109-19. doi:10.1016/j.psc.2013.01.011. Review. PubMed PMID: 23538081
Pomykala KL, Silverman DH, Geist CL, Voege P, Siddarth P, Nazarian N, St Cyr NM, Khalsa DS, Lavretsky H. A pilot study of the effects of meditation on regional brain metabolism in distressed dementia caregivers. Aging health. 2012 Oct 1;8(5):509-516. PubMed PMID: 23378856
Merrill DA, Siddarth P, Kepe V, Raja PV, Saito N, Ercoli LM, Miller KJ, Lavretsky H, Bookheimer SY, Barrio JR, Small GW. Vascular risk and FDDNP-PET influence cognitive performance. J Alzheimers Dis. 2013;35(1):147-57. doi: 10.3233/JAD-121903. PubMed PMID: 23380994
Lavretsky H, Newhouse PA. Stress, inflammation and aging. Am J Geriatr Psychiatry [in press]
Black DS, Cole SW, Irwin MR, Breen E, St. Cyr N, Nazarian N, Khalsa DS, Lavretsky H. Yogic meditation reverses NF-kappaB and IRF-related transcriptome dynamics in leukocytes of family dementia caregivers in a randomized controlled trial. Psychoneuroendocrinology. 2012 Jul 13. PubMed PMID:22795617.
Jain FA, Gitlin M, Lavretsky H. Rapid Response of Major Depressive Disorder and Comorbid Eating Disorder NOS to a Novel Meditation Intervention. Psychosomatics. 2012 Jul;53(4):401-2. PubMed PMID: 22748753.
Lavretsky H, Siddarth, P, Nazarian, N, St. Cyr, N, Khalsa, DS, Lin, J, Blackburn, E, Epel, ES, Irwin, MR. A pilot study of yogic meditation for family dementia caregivers with depressive symptoms: Effects on mental health, cognition, andtelomerase activity. Int J Geriatr Psychiatry. 2012 Mar 11. doi: 10.1002/gps.3790. PubMed PMID: 22407663.
Ercoli LM, W Small G, Siddarth P, Kepe V, Huang SC, Miller KJ, Lavretsky H, Bookheimer SY, Barrio JR, Silverman DH. Assessment of dementia risk in aging adults using both FDG-PET and FDDNP-PET imaging. Int J Geriatr Psychiatry. 2012 Mar 1. doi: 10.1002/gps.2816. [Epub ahead of print] PubMed PMID: 22383132.
Schneider B, Ercoli L, Siddarth P, Lavretsky H. Vascular burden and cognitive functioning in depressed older adults. Am J Geriatr Psychiatry. 2012 Aug;20(8):673-81. PubMed PMID: 21857219.
Lavretsky H, Alstein LL, Olmstead RE, Ercoli, LM, Riparetti-Brown M, St Cyr N, Irwin MR. Complementary Use of Tai Chi Chih Augments Escitalopram Treatment of Geriatric Depression: A Randomized Controlled Trial. Am J Geriatr Psychiatry. 2011 Oct;19(10):839-50.
Meeks TW, Vahia IV, Lavretsky H, Kulkarni G, Jeste DV. A tune in “a minor” can “b major”: a review of epidemiology, illness course, and public health implications of subthreshold depression in older adults. J Affect Disord. 2011 Mar;129(1-3):126-42. Review. PubMed PMID: 20926139; PubMed Central PMCID:PMC3036776.
Cho HJ, Lavretsky H, Olmstead R, Levin M, Oxman MN, Irwin MR. Prior depression history and deterioration of physical health in community-dwelling older adults- A prospective cohort study. Am J Geriatr Psychiatry. 2010 Jan 11. [Epub ahead of print] PubMed PMID: 20220581.Lavretsky H, Zheng L, Weiner MW, Mungas D, Reed B, Kramer JH, Jagust W, Chui H, Mack WJ. Association of depressed mood and mortality in older adults with and without cognitive impairment in a prospective naturalistic study. Am J Psychiatry. 2010 Feb 16. [Epub ahead of print] PubMed PMID: 20160005.
Lavretsky H, Siddarth P, Irwin MR. Improving depression and enhancing resilience in family dementia caregivers: a pilot randomized placebo-controlled trial of escitalopram. Am J Geriatr Psychiatry. 2010 Feb;18(2):154-62.
Mueller SG, Mack WJ, Mungas D, Kramer JH, Cardenas-Nicolson V, Lavretsky H,Greene M, Schuff N, Chui HC, Weiner MW. Influences of lobar gray matter and white matter lesion load on cognition and mood. Psychiatry Res. 2010 Feb 28;181(2):90-6.
Lavretsky H. Complementary and alternative medicine use for treatment and prevention of late-life mood and cognitive disorders. Aging health. 2009 Feb 1;5(1):61-78.
Lavretsky H, Siddarth P, Kepe V, Ercoli LM, Miller KJ, Burggren AC, Bookheimer SY, Huang SC, Barrio JR, Small GW. Depression and anxiety symptoms are associated with cerebral FDDNP-PET binding in middle-aged and older nondemented adults. Am J Geriatr Psychiatry. 2009 Jun;17(6):493-502.
Small GW, Siddarth P, Burggren AC, Kepe V, Ercoli LM, Miller KJ, Lavretsky H, Thompson PM, Cole GM, Huang SC, Phelps ME, Bookheimer SY, Barrio JR. Influence of cognitive status, age, and APOE-4 genetic risk on brain FDDNP positron-emission tomography imaging in persons without dementia. Arch Gen Psychiatry. 2009 Jan;66(1):81-7.
Cho HJ, Lavretsky H, Olmstead R, Levin MJ, Oxman MN, Irwin MR. Sleep disturbance and depression recurrence in community-dwelling older adults: a prospective study. Am J Psychiatry. 2008 Dec;165(12):1543-50.
Elderkin-Thompson V, Ballmaier M, Hellemann G, Pham D, Lavretsky H, Kumar A. Daily functioning and prefrontal brain morphology in healthy and depressed community-dwelling elderly. Am J Geriatr Psychiatry. 2008 Aug;16(8):633-42.
Lavretsky H. Neuropsychiatric symptoms in Alzheimer disease and related disorders: why do treatments work in clinical practice but not in the randomized trials? Am J Geriatr Psychiatry. 2008 Jul;16(7):523-7.
Lavretsky H, Zheng L, Weiner MW, Mungas D, Reed B, Kramer JH, Jagust W, Chui H, Mack WJ. The MRI brain correlates of depressed mood, anhedonia, apathy, and anergia in older adults with and without cognitive impairment or dementia. Int J Geriatr Psychiatry. 2008 Oct;23(10):1040-50.
Lavretsky H. Neuropsychiatric symptoms in Alzheimer disease and related disorders: why do treatments work in clinical practice but not in the randomized trials? Am J Geriatr Psychiatry. 2008 Jul;16(7):523-7.
Lavretsky H, Zheng L, Weiner MW, Mungas D, Reed B, Kramer JH, Jagust W, Chui H, Mack WJ. The MRI brain correlates of depressed mood, anhedonia, apathy, and anergia in older adults with and without cognitive impairment or dementia. Int J Geriatr Psychiatry. 2008 Apr 16.
Lavretsky H, Siddarth P, Kumar A, Reynolds CF 3rd. The effects of the dopamine and serotonin transporter polymorphisms on clinical features and treatment response in geriatric depression: a pilot study. Int J Geriatr Psychiatry. 2008 Jan;23(1):55-9.
Lavretsky H, Ballmaier M, Pham D, Toga A, Kumar A. Neuroanatomical characteristics of geriatric apathy and depression: a magnetic resonance imaging study. Am J Geriatr Psychiatry. 2007 May;15(5):386-94.
Lavretsky H, Nguyen LH. Innovations: geriatric psychiatry: diagnosis and treatment of neuropsychiatric symptoms in Alzheimer’s disease. Psychiatr Serv. 2006 May;57(5):617-9.
Lavretsky H, Park S, Siddarth P, Kumar A, Reynolds CF 3rd. Methylphenidate-enhanced antidepressant response to citalopram in the elderly: a double-blind, placebo-controlled pilot trial. Am J Geriatr Psychiatry. 2006 Feb;14(2):181-5.
Lavretsky H, Roybal DJ, Ballmaier M, Toga AW, Kumar A. Antidepressant exposure may protect against decrement in frontal gray matter volumes in geriatric depression. J Clin Psychiatry. 2005 Aug;66(8):964-7.
Lavretsky H, Kurbanyan K, Ballmaier M, Mintz J, Toga A, Kumar A. Sex differences in brain structure in geriatric depression. Am J Geriatr Psychiatry. 2004 Nov-Dec;12(6):653-7.
Lavretsky H, Ercoli L, Siddarth P, Bookheimer S, Miller K, Small G. Apolipoprotein epsilon4 allele status, depressive symptoms, and cognitive decline in middle-aged and elderly persons without dementia. Am J Geriatr Psychiatry. 2003 Nov-Dec;11(6):667-73.
Lavretsky H, Kitchen C, Mintz J, Kim MD, Estanol L, Kumar A. Medical burden, cerebrovascular disease, and cognitive impairment in geriatric depression: modeling the relationships with the CART analysis. CNS Spectr. 2002 Oct;7(10):716-22.
Lavretsky H, Bastani R, Gould R, Huang D, Llorente M, Maxwell A, Jarvik L;UPBEAT Collaborative Group. Unified Psychogeriatric Biopsychological Evaluation and Treatment. Predictors of two-year mortality in a prospective “UPBEAT” study of elderly veterans with comorbid medical and psychiatric symptoms. Am J Geriatr Psychiatry. 2002 Jul-Aug;10(4):458-68.
Lavretsky H, Kumar A. Clinically significant non-major depression: old concepts, new insights. Am J Geriatr Psychiatry. 2002 May-Jun;10(3):239-55. Review.
OPTIMUM: Optimize Your Treatment For Depression
Study Detail

OPTIMUM is a research study designed to test medications for older adults with depression suffering from treatment resistant depression. The study is designed to test which medications work best and are safest for older adults.
Older adults experiencing major depression that persist despite treat,ment with two or more standard antidepressants may be eligible.
ELIGIBLE:
Age 60 years and older
Treatmetn resistant depression- major depression (PHQ-9=>6) who failed two or more trials of antidepressants.
EXCLUDED:
Dementia; Unstable medical illness; unable to take medications prescribed in the OPTIMUM study (aripiprazole, Bupropione, Lithiuml Nortriptyline)
In order to refer a patient, please email: LateLifeWellness@mednet.ucla.edu or call 310 794-4619 0r 310-206-5240
Project: Optimize Your Treatment For Depression
OPTIMUM for Providers
Study Detail
OPTIMUM: Optimizing Outcomes of Treatment-Resistant Depression in Older Adults
What do you do when your older adult patient with depression has failed not just the first antidepressant, but the second as well? Which next step is best for them?
Help us find out, in the OPTIMUM study:
A pragmatic study:
- comparing risks and benefits of different treatment options in real world clinical settings
- for older adults whose depression has not improved with first line treatment
A large scale study:
- Our academic partners include medical researchers at the University of Pittsburgh, Columbia University, the University of California, Los Angeles, and the Centre for Addiction and Mental Health in Toronto.
- By partnering with you and other providers, we aim to enroll 1,500 older adults in the study
Our goal is to support you in providing excellent care to your patients with treatment-resistant depression:
- During the study – We will check in with participants often, keep you updated on their progress, and make evidence-based medication recommendations.
- In the future – With your help, we will fill a major gap in the evidence and provide clinicians with new information to provide optimal care to older adults.
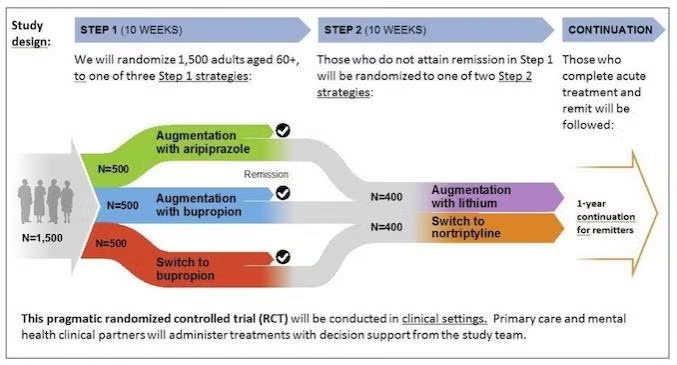
PCORI Inclusion criteria:
a) Men and women aged 60 and older, with equal proportions aged 60-70 and 70+.
b) Current Major Depressive Disorder (MDD), single or recurrent, as diagnosed by DSM-5 criteria.
c) Failure to respond adequately to two or more antidepressant treatment trials of recommended dose and length (at least 12 weeks).
d) PHQ-9score of 6 or higher.
PCORI Exclusion Criteria:
a) Inability to provide informed consent.
b) Dementia, as defined by Short Blessed >10 and/or clinical evidence of dementia. Patients screened out due to possible dementia will be referred to a local Memory Clinic or back to their clinician for evaluation to clarify the presence or absence of dementia.
c) Lifetime diagnosis of bipolar I or II disorder, schizophrenia, schizoaffective disorder, schizophreniform disorder, delusional disorder, or current psychotic symptoms, as diagnosed by the MINI. A recommendation for psychiatric referral will be made in these cases.
d) High risk for suicide (e.g., active SI and or current/recent intent or plan) and unable to be managed safely in the clinical trial, such as unwilling to be hospitalized).Urgentpsychiatric referral will be made in these cases.
e) Contraindication to proposed study medications, as determined by study physician includinghistoryof intolerance or non-response to proposed medications.
f) Non correctable, clinically significant sensory impairment (e.g.,cannothear well enough to cooperate with interview).
g) Unstable medical illness, including delirium, uncontrolled diabetes mellitus, hypertension, hyperlipidemia, or cerebrovascular or cardiovascular risk factors that are not under medical management. This will be determined based on information from the patient’s personal physician’s and study physician clinicaljudgement. Referral to the patient’s personal physician or to a general practitioner will be made in these cases.
h) Moderate to severe substance or alcohol use disorder, as determined by study physician. Referral to appropriate treatment will be made in these cases.
For more information, please contact:
Helen Lavretsky, MD, Principal Investigator
hlavretsky@mednet.ucla.edu
310-794-4619
Project: Optimum for Providers
Participate
Later Life Depression, Stress and Wellness Research Program Research Study Participation Opportunities
Below are listed the current opportunities for participation in research studies within this group. Click on the title to read more detail.
- Art and Well-Being Study [flyer]
- Effects of COVID-19 on the Brain [flyer]
- Online Wellness Interventions for Brain Connectivity and Cognition Improvement [flyer]
- OPTIMIZAR SU TRATAMIENTO PARA LA DEPRESIÓN [flyer]
- OPTIMUM for Providers [flyer], [flyer]
- OPTIMUM: Optimize Your Treatment For Depression [flyer]
Training
Educational Opportunities and Affiliated Programs
Elective clinical research rotation for medical students at UCLA – follow the links in our Medical Education section for more information
Summer Research Fellowship for medical, undergraduate, and graduate students (applications solicited prior to the month of January of each year)
Geriatric psychiatry and psychology fellowship program
Resources
Useful Resources
HEALTHFLIX
Andrew Weil Center for Integrative Medicine
The Sound of Healing | Vital Signs
Vital Signs Issues
Population Behavioral Health
Behavioral Health Associates
East west medicine resources
Self Help
For people who can’t participate in the studies, exercise with a friend every day. Get a video or DVD about Tai Chi, or simply try creating your own slow-motion exercises. Several good books are available:
- Living Longer Depression Free: A Family Guide to Recognizing, Treating, and Preventing Depression in Later Life by Mark D. Miller, Charles F. Reynolds III.
- Resilience and Aging: Research and Practice by Helen Lavretsky
- Late-Life Mood Disorders edited by Helen Lavretsky, Martha Sajatovic, Charles F. Reynolds III.
- The Use of Natural Products and Supplements in Late-Life Mood and Cognitive Disorders by Taya C. Varteresian, David A. Merrill, Helen Lavretsky
- Alzheimer’s: A Caregiver’s Guide and Sourcebook, by Howard Gruetzner
- The 36-Hour Day: A Family Guide to Caring for People with Alzheimer Disease, Other Dementias, and Memory Loss in Later Life, by Nancy L. Mace, Peter V. Rabin
Useful Websites
The Family Caregiver, www.thefamilycaregiver.org
Senior Services, www.seniorservices.org
MedlinePlus, www.nlm.nih.gov/medlineplus/depression.html
Depression and Bipolar Support Alliance, (800) 826-3632, www.dbsalliance.org
UCLA Health Integrative Medicine, https://www.uclahealth.org/integrative-medicine
Collaborations
Collaborative projects are established with the Intramural Research Programs at UCLA:
- Memory and Aging Center (Dr Gary Small- Director) www.memory.ucla.edu
- Cousins Center for Psychoneuroimmunology (Dr Michael Irwin-Director) www.cousinspni.org
- Mindful Awareness Reearch Center (Dr Susan Smalley-Director) marc.ucla.edu
- Alzheimer’s Disease Center (Dr Jeffrey Cummings- Director) www.adc.ucla.edu
- Geriatric Neuropsychology (Dr Linda Ercoli- Director)
- Center for Addictive Behavior (Dr Edythe London- Director) www.semel.ucla.edu/cab
- Consortium for Neuropsychiatric Phenomics (Dr Robert Bilder- Director) www.phenomics.ucla.edu
- Center for Neurobehavioral Genetics, Southern California Genotyping Consortium (SCGC) (Dr Nelson Freimer- Director) www.semel.ucla.edu/neurogenetics/
Extramural Collaborations:
- The Late-Life Depression Research Center at the University of Pittsburgh (Dr Charles F. Reynolds- Director) www.wpic.pitt.edu/research/depr
- The Center for Addiction and Mental Health, at the University of Toronto (Dr Bruce Pollock- Vice President) www.rotman-baycrest.on.ca/
- Alzheimer’s Prevention Foundation www.alzheimersprevention.org
- American Association for Geriatric Psychiatry www.aagponline.org
Additional Resources:
Depression in Late Life: Not A Natural Part Of Aging
A Different Way to Deal With Depression
Kirtan Kriya p.1
Care when you need it, wherever you are
Self-Care Tips to Boost Immunity
People
-

Helen Lavretsky, MD
Director -

Pauline Wu, DO
Faculty -

Jason Jalil, MD
Faculty -

Stephen Chen, MD
Faculty -

Linda Ercoli, PhD
Faculty -

Katherine Narr, PhD
Faculty -

Lisa Kilpatrick, PhD
Faculty -

Sarah Nguyen, MD
Faculty -

Hanadi Ajam Oughli, MD
Faculty -

Prabha Siddarth, PhD
Statistician -

Courtney Sheen
Research Associate -

Grace Hemphrey
Research Associate
Volunteers:
- Devin Patel
- Carlos Landaverde
- Vaidehi Ramanarayanan
News
2026
03/21/2026 UCLA Health Brain Health Summit March 21, 2026
03/20/2026 UCLA Health Brain Health Summit March 20, 2026
01/09/2026 ISCR Webinar Dec 2025 Mind-Body therapies, Resilience and Brain Helath in Aging
2025
12/18/2025 Managing Cognitive Impairment: Integrative Approaches in Geriatric Psychiatry
12/09/2025 Exploring the Mind-Body Connection: Dr. Helen Lavretsky on Tai Chi, Meditation, and Brain Health
11/24/2025 Activities for Cognitive Health
11/06/2025 Breathe: Reducing stress can help your brain
09/22/2025 Breathwork for Longevity: Reverse Biological Aging & Boost Mental Health
09/09/2025 Yoga isn’t just for flexibility. It may also protect brain health
08/25/2025 Psychiatry and Spirituality: Exploring the Intersections of Meaning and Mental Health
08/25/2025 Return of the Soul: The Role of Spirituality in Mental Health
07/07/2025 BCA – Caregivers of Persons with Psychiatric Disorders and Dementia
05/19/2025 Teaching Resilience at the 2025 APA Annual Meeting
04/25/2025 Even Low-Key Exercise Is Fantastic for Your Brain
03/30/2025 How to use your voice to reduce your stress and feel calmer
03/28/2025 Post-Acute Sequelae of COVID-19 Infection Presenting With Neuropsychiatric Symptoms: Diagnosis and Management
03/21/2025 Cultivation of Mind-Body-Brain-Soul Connections withTechnology?
02/04/2025 Weekend Warriors Can Still Reap Brain Health Benefits from Exercise, Study Says
01/22/2025 Meditation, art and nature: Neuroimaging reveals distinct patterns of brain activation
01/19/2025 Your brain on art, nature, and meditation: a pilot neuroimaging study
01/07/2025 Boost brain health with daily lifestyle practices
01/01/2025 How to calm your mind with breathing, according to science
2024
11/21/2024 Brain Medicine
11/21/2024 Chronic Inflammation Is Both Dangerous and Very Common—Here’s How to Know If You Have It
11/20/2024 UCLA’s Lavretsky Revolutionizes Brain Health Research
08/15/2024 Yoga for the brain: How it helps cognition, may protect against decline
08/08/2024 Cognitive health isn’t just about the mind
08/02/2024 Mental Health in Later Life with Dr. Helen Lavretsky
07/24/2024 Myalgic Encephalomyelitis/Chronic Fatigue Syndrome After SARS-CoV-2 Infection
07/17/2024 How to (gently) talk to aging parents about downsizing and decluttering
07/07/2024 Older Women Are Different Than Older Men. Their Health Is Woefully Understudied.
06/16/2024 Older women are being significantly shortchanged by medical research
05/29/2024 Polypharmacy in Older Adults
05/07/2024 Geriatric Psychiatry: Life Is Not Over at 65
04/04/2024 Yoga provides unique cognitive benefits to older women at risk of Alzheimer’s disease, study finds
04/03/2024 Breathing not-so-easy: Can meditation and ice baths really set your mind and body free?
03/27/2024 Practicing Yoga Can Help Prevent Alzheimer’s Disease
02/28/2024 Yoga Brings Brain Benefits to Women at Risk for Alzheimer’s
02/26/2024 Kundalini yoga bolsters cognitive health among older women at risk of Alzheimer’s disease
01/24/2024 Breathing Matters | UCLA Neuroscience Research Theme Event
01/08/2024 Yoga May Be Even Healthier Than You Thought. Here’s Why
2023
12/27/2023 Integrative Therapies for Brain Health and Aging
12/15/2023 2023 AAGP Brain Health Summit- moderated by Dr Helen Lavretsky
11/30/2023 Dementia Untangled 11/20/2023 Dr. Helen Lavretsky Interview – Human Kind
11/03/2023 2023 Annual UCLA Integrative Medicine Conference
09/26/2023 Life-Course Brain Health as a Determinant of Late-Life Mental Health: American Association for Geriatric Psychiatry Expert Panel Recommendations
09/20/2023 Tai chi as mind-body medicine? A UCLA Health psychiatrist aims to take the practice nationwide
08/09/2023 Couples’ Guide to Keeping Your Heart Healthy
08/03/2023 A new understanding of the power of yoga
07/28/2023 This yoga may benefit women with high risk of Alzheimer’s disease
07/26/2023 Kundalini yoga may be beneficial for older women with Alzheimer’s risk factors
07/20/2023 Yoga may improve cognitive function in older adults at risk for decline
07/11/2023 Integrative Therapies for Older Adults
03/06/2023 NFL star Aaron Rodgers went on a darkness retreat. What’s that?
02/23/2023 Is long COVID a neurological disease? Scientists are doing more research
02/14/2023 Long COVID Now Looks like a Neurological Disease, Helping Doctors to Focus Treatments
01/31/2023 Depression, poor mental health in young adults linked to higher cardiovascular risks
01/31/2023 What COVID-19, mental health and aging have in common
2022
10/06/2022 The vital crosstalk between breath and brain
08/24/2022 Patient Education Webinar: Integrative solutions for neuropsychiatric symptoms with Dr. Lavretsky
07/26/2022 Fears of more long COVID, a ‘mass disabling event’ as variants rip through California
06/29/2022 Life’s Essential 8: Updating and Enhancing the American Heart Association’s Construct of Cardiovascular Health: A
Presidential Advisory From the American Heart Association
02/14/2022 Desperate Americans Are Going Abroad for Unproven Long COVID Cures
01/11/2022 Semel Grand Rounds, 2022-01-11, Dr. Helen Lavretsky, Dr. Joann Elmore & Dr. Elyse Singer
2021
10/28/2021 Could Breastfeeding Help Women Keep Their Smarts as They Age?
10/23/2021 Breastfeeding May Help Prevent Cognitive Decline – Neuroscience News
10/23/2021 Many Covid patients have memory problems months later, new study finds
10/23/2021 New study suggests that breastfeeding may help prevent cognitive decline — ScienceDaily
10/14/2021 Adele tried sound baths for stress: What are they? Do they help? Experts explain
07/23/2021 What Will the Future of Alzheimer Disease Treatment Look Like?
07/19/2021 Addressing the Cognition Crisis in Our COVID-19 World
06/02/2021 Medical Research: Prerecorded – Panel 4 – Presentation 5
05/19/2021 Integrative Mental Health in The Time of COVID
04/12/2021 The latest interview for Forbes magazine about climate change and impact on older adults
03/24/2021 Feeling Lucky? Convergence Mental Health as a Mechanism for Serendipitous Innovation
02/02/2021 Mental Health Plays a Role in Treating and Preventing Heart Disease
01/07/2021 Disaster Stress, Mental Health, and Aging: How Mind-Body Therapies Can Build Resilience
01/05/2021 Convergence Mental Health
2020
11/04/2020 UCLA Integrative Psych, 2020-11-04, SARS-CoV-2 : Complementary & Integrative Treatments Update
09/30/2020 An Opportunity for Growth
09/28/2020 Mind, Consciousness, and Well-Being
08/31/2020 Seniors With Depression Show Resilience in Face of Pandemic
07/08/2020 The Upside and Downside of Religion, Spirituality, and Health
06/29/2020 How are older adults with Depression experiencing the COVID-19 pandemic?
06/16/2020 Get the latest information from the CDC about COVID-19
06/10/2020 UCLA/Egoscue Interview
05/19/2020 The COVID-19 Honeymoon Is Almost Over 05/03/2020 Yoga Scholars Pgimer
04/10/2020 New research on how yoga improves memory and focus
03/16/2020 COVID-19 Information
03/05/2020 What’s The Deal With Sound Baths And Do They Actually Work?
02/11/2020 UCLA Newsroom
2010 – 2019
08/16/2019 Memory – How Yoga Improves Cognitive Functioning
03/27/2018 Exploring Scientific Evidence for Sound Healing at Integrative Medicine Conference
02/22/2018 Resilience in the context of ageing with Dr. Helen Lavretsky
02/20/2018 Resilience in the Context of Ageing with Helen Lavretsky, MD, MS
10/12/2017 Dr Lavretsky presents at the 5th Body, Mind and Life Institute in Dharamsala, India, October 4-6, 2017
09/13/2017 I tried to cure my anxiety by hallucinating. Interview by the Cosmopolitan
08/10/2017 OPTIMUM study featured by UCLA Bruin paper
08/08/2017 Cognitive enhancement with yoga
05/25/2017 5 Ways We Can Begin Taking Preventative Measures Today To Improve Brain Fitness
04/01/2017 How Spirituality Benefits Older Adults
03/01/2017 Mantra Meditation in LAYOGA
02/23/2017 LA times article on the benefits of yoga with Dr Lavretsky
01/20/2017 Comparison of Yoga or MEmory training in older adults
01/17/2017 A randomized controlled trial of Kundalini yoga in mild cognitive impairment.
01/06/2017 Helen Lavretsky, M.D. featured in Psychiatric News
12/13/2016 Neurochemical and Neuroanatomical Plasticity Following Memory Training and Yoga Interventions in Older Adults with
Mild Cognitive Impairment.
12/13/2016 The Neural Mechanisms of Meditative Practices: Novel Approaches for Healthy Aging.
09/30/2016 CNN health news today: Late life treatment resistant depression
09/28/2016 Dr Lavretsky featured in Psychiatric Times- Path to personal and professional peace and fulfillment.
09/28/2016 Natural Supplements and Vitamins for Treatment and Prevention of Dementia and Cognitive Decline
09/28/2016 Treatment resistant depression in Psychiatric Times
09/26/2016 Dr. Weill blog
08/30/2016 A UCLA team of neuroscientists found that a three-month course of yoga and meditation helped minimize the cognitive
and emotional problems that often precede Alzheimer’s disease and other forms of dementia.
08/30/2016 All to do about aging
08/30/2016 PCORI Board Approves $40 Million for Improving Treatment Options for Depression
08/09/2016 Podcast: Surprisingly Awesome #18 Yoga
02/09/2016 Top-down Plus Bottom-up Integrative Treatments in Psychiatry
01/07/2016 New England J Medicine Journal Watch Psychiatry Top Stories of 2015
02/27/2015 The Benefits of Yoga and Meditation for Alzheimer’s and Dementia
11/17/2014 Dr. Helen Lavretsky writes new book to help aging populations cope with stress
05/24/2013 Mindful exercise and mental health
05/13/2013 Mindful Exercises and Meditation: Neurobiological Effects
02/27/2013 Late-Life Mood Disorders
02/27/2013 The Use of Natural Products and Supplements in Late-Life Mood and Cognitive Disorders
07/30/2012 Media Showcase Benefits of Yoga to Reduce Stress
07/30/2012 Yoga for Cancer Patients and Caregivers
07/27/2012 KABC Reports the Benefits of Kirtan Kriya Meditation for Caregivers
07/27/2012 ScienceDaily Features that Yoga Reduces Stress
03/25/2011 Tai Chi May Lift Depression in Seniors
09/03/2010 Resilience, Stress, and the Neurobiology of Aging
Event
UCLA Health Brain Health Summit
Friday, March 20, 2026 – 7:15am to Saturday, March 21, 2026 – 5:00pm
UCLA Health Brain Health Summit Program
Day 1 Speaker Biographies – UCLA Health Brain Health Summit
Day 2 Speaker Biographies – UCLA Health Brain Health Summit
Videos
UCLA Health Brain Health Summit March 20, 2026
UCLA Health Brain Health Summit March 21, 2026

Summary:
The UCLA Health Brain Health Summit brings together research, policy, and community voices to advance brain health across California, the US, and globally.
Date and Time:
03/20/2026 — 03/21/2026 7:15 AM – 5:00 PM
Location:
UCLA Meyer and Renee Luskin Conference Center
425 Westwood Plaza, Los Angeles, CA 90095
Overview:
Welcome to the UCLA Health Brain Health Summit!
The UCLA Health Brain Health Summit will be held March 20–21, 2026, at the UCLA Luskin Center and will unite researchers, clinicians, policymakers, and communities to advance brain health across California, the US, and globally. In an era marked by climate disasters, social upheaval, and a rapidly aging population, brain health must be recognized as a fundamental public health priority essential to individual resilience and societal well-being. Evidence-based interventions can protect function, strengthen resilience, and reduce long-term effects.
Brain health encompasses cognitive, emotional, neurological, and social functioning across the lifespan, from early development through older age. While the brain is shaped by environmental, lifestyle, and social factors, research shows that prevention, early detection, and evidence-based interventions can protect function, strengthen resilience, and reduce long-term decline. Yet access to these strategies remains uneven, particularly for underserved communities.
Brain skills such as creativity, critical thinking, adaptability, and resilience are increasingly vital in a rapidly changing world shaped by technological advances and shifting workforce demands.
Through interdisciplinary dialogue and community engagement, the UCLA Brain Health Summit will examine practical approaches to measuring brain health, translating research into action, and advancing community-based and policy solutions to address the growing brain and mental health crisis.
Sponsors:
